A human being has between 100.000 and 150.000 hairs. About 150 to 200 hairs are implanted per square centimetre. The total length of all these hairs is 3 kilometres in the case of short-haired men, and 30 to 50 kilometres in the case of long-haired women …
Our hairs grow at a speed of 1 centimetre per month. Their diameter is about one tenth of a millimetre.
We loose 40 to 50 hairs per day, but we get the same number of new hairs.
Every follicle produces between 20 and 30 hairs, in a cycle which lasts three and a half years on average :
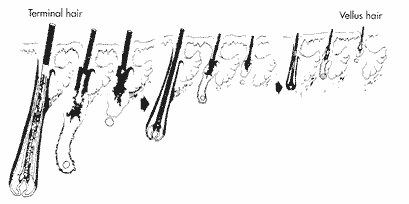
– The anagen phase (85%) during which the hair grows (2 to 5 years).
– The catagen phase (1%) during which the hair no longer grows, but still remains in place (a few days).
– The telogen phase (14%) during which the hair is detached from the scalp and falls out (2 to 3 months).
There is a period of inactivity between two consecutive cycles. This lasts a few months.
Women and children have a higher proportion of hair in the anagen phase than men.
As commonly known, the hormonal situation of women has an impact on their hair cycle : the phase of rest lasts longer during pregnancy, as a result of which the number of hairs will temporarily increase. After giving birth, however, there is an increased loss of hair.

The lifetime of some of a man’s hair-roots (on the forehead and the crown) is genetically shorter as a result of shortened cycles, which in their turn result from the influence of the male hormone (testosterone) and from the number of receivers of this hormone on the hair-roots.
his causes hair-roots to die, with no new hairs being added. This loss of hair is called androgenetic alopecia. It causes a baldness which is genetically determined and which is therefore transmitted from one generation to the other.
The hairs in the hippocratic area, i.e. the area between the neck and the temples, have less testosterone-receivers and are therefore less subject to this hormone. As a result of this, they have a normal lifetime and these hairs can last a whole life.
It is therefore in this area that future implants will be taken. Since they take their genetic information with them, they can be moved without any impact on their original lifetime.
Remark : women, too, can suffer from androgenetic alopecia, but in their case it will be spread over the entire skull.
The classification of Hamilton distinguishes between seven levels of baldness with men.
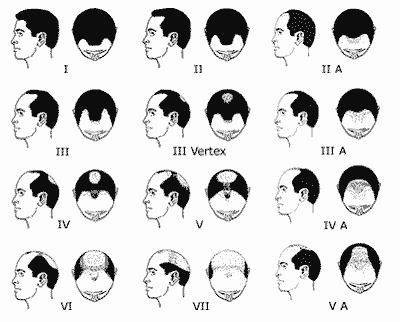
Hereditary baldness is the most frequent cause of loss of hair.If this cause is excluded, all forms of excessive loss of hair or of hair becoming thinner, must be taken seriously.
– Child-birth : the loss of hair will decrease during pregnancy, as a result of which there will be an increased loss of hair during the first months after having given birth .
– A period of increased body-temperature or serious infection, as well as major surgery can be followed by a period of three months with increased loss of hair.
– Illnesses of the thyroid gland.
– Low-protein diets and a lack of magnesium, calcium, potassium, zinc, iron, vitamins or mineral salts (watch out for unbalanced diets!)
– Certain drugs and anti-cancer treatments.
– Contraceptives when the woman has a hereditary predisposition to baldness.
– Alopecia areata : an illness of the scalp which makes the hairs fall out in bundles.
– Mycosis of the scalp : an infection of the scalp which is caused by a fungus.
– Repeated aggressive hair-treatments (colouring, decolorisation, tight hair-knots, uncurling) can make the hairs fragile and cause them to break .
– Grave stress-factors (e.g. mourning, emotional shocks, surgery)
– Trichotillomania : a nervous twitch which makes people pull out their hairs.
Most of these affections can be treated. But when the hair has been affected in an irreversible manner, then a hair-transplant is the only natural solution.
The trichogram :
About 50 hairs are removed from different parts of the scalp (the scalp should not have been washed since 3 or 4 days).
These hairs are then examined under a microscope or under a microfilm-reader in order to determine which percentage of the hairs are in each of the three phases of the cycle.
The percentage of hairs in the anagen phase is higher with women and children than with men.
In order to establish the degree by which loss of hair is compensated (and, therefore, in order to assess the patient’s situation), and in order to determine at what rate baldness will progress, the proportion of anagen hairs (which are in their growing-phase) is compared to the proportion of telogen hairs (which are about to fall out).
The trichogram is obviously an essential diagnostic tool.
The photo-trichogram.
An area of the scalp, a square centimetre in size, is shaven and macroscopic pictures are taken. A second set of pictures, taken five days later, will allow to establish the percentage of new hairs. In order to obtain an even more precise idea of the rate at which new hairs grow, one can review the situation again after one month.
Analysis of the hair under a microscope
When the hair is exceptionally fragile, which could indicate a fungous, a bacterial or a viral infection.
Analysis of the hair in a laboratory
This serves to determine hereditary defects of the hair’s protein composition, as well as changes caused by drugs or by heavy-metal contamination.
Biopsy of the scalp
In the case of exceptional loss of hair, a biopsy can give additional information as to the reason why the hairs break off.
Is hardly used at all.
Les traitements médicaux : Food-supplements, lotions and vitamins (Biotine, Bépanthène, vitamin B,…) can overcome most affections of the scalp.
Minoxidil-lotion (Regaine) : This is the only local treatment, effective in 60% of cases. When applied twice daily over a long period, it can slow down the loss of hair. It is recommended to young men only. As soon as the treatment is halted, the loss of hair will continue as before.
Finasteride (Propecia) : This drug, which has been used for many years in the treatment of hypertrophy of the prostate, halts the progress of baldness with more than 80% of the patients.
In 66% of all cases, there is even renewed hair-growth !
Dermography (tattoos), can sometimes offer an interesting alternative. The scalp is coloured to create the impression that it is covered with hairs …

Their advantages and disadvantages are well known. It is up to everyone to judge …
Artificial : in the past, different kinds of synthetic hairs were implanted. However, the risks of rejection, allergic reactions and infections were very big.
Own hairs : this methode makes it possible to spread the ‘hair capital’ in a well-balanced manner. One avoids bald spots and one can gradually move from dense to less dense hair, which still covers the entire skull.
This technique has been perfected a lot over the recent years.
The capillary auto-transplant was carried out for the first time in 1938.
It was further developed and systematized by professor Orentreich.
Until the late nineteen-eighties, big grafts (with a diameter of 4 to 6 millimetres) were used. These were implanted in rows next to one another, which resulted in a doll’s head appearance.
In order to avoid this, the technique started to use mini-transplants (small parts of the scalp, each with only a few hairs). This was a substantial improvement compared to the previously used technique.
As the technique was developed further still, doctors logically ended up in the other extreme of micro-transplants whereby individual hairs were transplanted one by one, in an effort to reach the aesthetically ideal image. Individual transplants do indeed have a very natural look, but the result also looked very thin.
The next step was that analysis under a magnifying glass showed that hairs are not implanted in the skin one by one, but in groups of 1 to 4 hairs, the so-called follicular unit.
Nowadays, these follicular units are kept as mother nature has given them to us. They are transplanted in their natural state, the only difference being that micro-transplants are used for the frontal hair-line, whereas micro-transplants with 2 to 4 hairs are used on the rest of the head. This way of working contributes to a well-balanced hair-density.
The technique to remove the hair has been improved as well, the strip-method having replaced the punch-method. It is now possible to perform several sessions. All that is left is a narrow scar at the back of the skull, which is covered by hair anyway.
The hairs are removed in narrow strips at the back of the skull. These strips are then meticulously cut into tiny transplants. This allows for the follicular units to be split and to be sorted by number of hairs per unit. The area where the strips have been removed is closed which leaves only a very fine skar, which will be covered by hair anyway.
The follicular units are then implanted one by one in micro-incisions which are made in the scalp by means of a micro-bistouri.
The pattern and the angle of these incisions is identical to those of the original implant. Since only micro-incisions in the scalp are made, the blood-circulation is not affected. This gives the micro-transplants an optimal chance to survive and allows for a maximum hair-density to be obtained. It goes without saying that this density can only be obtained if the operating team is extremely skilled in this kind of operation..
During an intervention which respects the necessary safety margins for any kind of aesthetic operation, up to 5000 transplants can be implanted per session. This corresponds to between 10.000 and 12.500 hairs.
Because this implant-technique is so remarkably precise, it even allows for hairs to be added on parts of the head where there are still hairs.
The operation can be repeated several times. This depends on the area which needs to be covered with hair, and on the hair-density which is wished.
Because of the optical effect, larger bald areas than before can be covered. The patient’s hair capital can thus be optimally exploited. And the effect lasts a lifetime ! The aim is obviously not to regain the same quantity of hair as when one was young, but to have the same volume of hair as a man of the same age who has no exceptional hair-loss.
This technique has seen an enormous boom in the past few years, for it uses our own hairs and thus creates hair that can be cut and modelled in the same manner as the original hair.
The ideal recipe therefore is : natural (micro-transplants with one hair, at the front), concentrated (micro-transplants with 2 to 4 hairs, behind) and manifold (lots of transplants can be made during a session).

The FUT procedure involves removing a strip of tissue from the base of the skull, from which the grafts are then extracted. This extraction results in a fine-line scar that may be visible if the hair is worn short.
In the FUE procedure, hairs are removed using a manual or motorised punch of 1 mm or less in diameter, resulting in small apertures that heal to leave virtually invisible white dots. The grafts extracted, each containing 1 to 4 hairs, are then checked by assistants to ensure they are suitable for replantation. The donor area is quick to heal.
Implantation is performed in the same way as in the conventional FUT technique, under local anaesthetic, via micro-incisions made using fine needles or blades. Both techniques therefore achieve the same result in the recipient area. The only difference is the subsequent appearance of the donor area.
Compared with traditional hair transplants, extraction using the FUE procedure is particularly recommended for :
– Patients with short hair, or who may decide to shave the nape of their neck in the future.
– Patients who require only a small transplant (to cover only a small area or to correct a cosmetic surgery scar or a previous implant).
– Patients seeking beard or eyebrow transplants, as it offers a very elegant solution to a number of cosmetic imperfections.
– It leaves few or no scars (tiny white dots that are completely concealed by the hair).
– Hair can be removed from a much broader area than under the FUT procedure, and transplants may be performed on patients with thin hair in donor areas.
– Body hair, such as chest or beard hair (for males), can be used.
– Patients experience more prolonged discomfort when lying on their stomach than patients who have undergone FUT, and the procedure itself takes longer.
– The head is usually shaved completely, although in some cases it is possible to shave the head partially in strips of between 1 cm and 2.5 cm in width.
– This technique is not suitable for patients with curly hair.
– Patients must dye any grey hairs prior to the procedure.
The first consultation is absolutely necessary.
It gives the patient the opportunity to talk about his problem and to explain which result he wants to have.
During this consultation, the patient’s medical and capillary antecedents (personally and in the family) are examined.
The patient’s scalp is examined at the donor zones and at the recipient sites. Diagnostic examinations (trichogram etc.) may be carried out as well. They enable the doctor to assess the future evolution of baldness and to analyse possible treatments.
Once this has been done, the doctor and his patient can discuss which treatment strategy to use, based on the collected information.
Since no one has an unlimited hair capital, one has to use it parsimoniously.
It is therefore important to anticipate future loss of hair and not to behave in a reactive manner, which would always stay one step behind the progressing baldness. The operation will only be a success if the result lasts for many years, making the first operation at the same time the last one …
The doctor will explain the result that can reasonably be expected. He will also discuss the advantages, the disadvantages and the costs. His explanation must be clear, complete and fair. It should also give an answer to the patient’s questions, and it must take into account the patient’s specific situation.
This discussion will build the trust between the doctor and his patient, an absolute prerequisite before any aesthetic surgery is undertaken.
Ample time to reflect must be given before the intervention is actually carried out.

It is recommended that someone should accompany the patient to his home.
Also, in view of the – minimal – risk of a drop in the blood-pressure, someone should be near the patient during the first night after the surgery.
A bandage is usually not needed.
This means that the patient can continue his professional life and his social life without any interruption
The only visible sign of the operation can be tiny scabs in the recipient site. These scabs will fall out by themselves after 2 to 4 weeks. If the patient wishes so, they can even be removed much quicker.
The doctor will prescribe a disinfecting lotion for the patient to use during the first few days.
It is possible that there is some minimal bleeding in the donor zone or in the recipient site during the first two nights.
There is no post-operative pain as such. The only thing that may occur is a sensation of a tensed scalp during the first 24 hours.
From the third day onwards, the forehead sometimes swells. This can also occur at the eyelids. However, this swelling disappears on the fifth day. And, anyway, it can be avoided if preventive medicine is taken.
The patient may already shampoo his hair from the day after the operation onwards. eHowever, he has to do it softly, staying clear from the zones that have been treated. These can be rinsed but should not be touched.
After 3 days, which is after 10 to 15 days, one is again allowed to shampoo the entire scalp.
Around the fourth week, some of the hairs that have been implanted will fall out. This will do no harm, since the root of these hairs remains intact. This means that new hairs will grow from these roots between the second and the fifth month.
The hairs that do not fall out, will immediately start to grow again, at the normal rate of one centimetre per month. During the period in which the hairs will again begin to grow, epidermal cysts may occur. These result from an irritation of the skin which is caused by new hairs not immediately getting through the scalp. Another possible issue is when the donor zone temporarily becomes over-sensitive.
The change takes place very gradually over a period covering several months. This makes it go unnoticed by the people around you. It makes the intervention a very discreet one indeed.
The final result can be assessed after 6 to 12 months.
Remark : in case there has been a treatment with Regaine and/or with Propecia before, this can be continued during this entire period.

Yes. The capillary micro-transplant technique makes it possible to implant hairs across the bald parts of the head in such a way that an optical impression of a full head of hair is created. Since the patient’s own hairs are used, there is no rejection. The obtained result is therefore lasting. And, finally, the transplanted hairs retain their shape, colour and texture.
– JI do not want to look like my bald father (or mother).
– I have lost a lot of hair and therefore I look older than my age.
– It bothers me that people notice that I am becoming bald.
– My reflection in the mirror is different from the way I feel.
– I want to have an ideal head of hair, in order to please better.
The solution is likely to consist of placing follicular microtransplants in between the old transplants, in order to make the latter disappear in the mass of transplanted hairs.
In some cases, it may be necessary to remove the old and coarse transplants. But then at least the hairs can be recovered from them.
Only the local anaesthesia hurts a little, similar as the one used by your dentist. There is hardly any pain after the surgery. The only feeling is that of a tense scalp. Although the doctor will prescribe a painkiller, it will usually not even be necessary to take it.
The scar in the donor zone is narrow as such, and it will be hidden by the hairs anyway. In the recipient site, no scars are visible at all thanks to the micro-incision technique.
This can already be done from the day after the operation onwards. It is even recommended to do it on a daily basis. This will make the scabs disappear quicker.
How many micro-transplants and how many sessions are needed ?
This depends on the size of the bald spots. Also, one must keep in mind that zones which still have hairs in them now, but which may loose these hairs in the next few years, must receive implants as well.
On average :
– 400 to 600 transplants are needed for the crown or for the temples.
– 1.000 transplants are needed for a partial baldness across the frontal and the upper part.
– and from 1.500 transplants for widespread baldness.
Thanks to the follicular micro-transplants, the result looks very natural from the first session onwards.
The number of sessions depends solely on the density of hair which the patient wants.
No, since the patient’s own hairs are transplanted.
Most patients resume their professional activities already on the day after the intervention.
An oedema can sometimes occur on the forehead. However, it is only very small. If one wants to be totally discrete about the intervention, it may be necessary to interrupt one’s activities for a few days. Anyway, taking appropriate medicine prior to the intervention will avoid most of this swelling.
Although there is no such thing as zero risk,it is clear that the risks are kept as low as possible by having an experienced and competent team, which uses the equipment which is required to guarantee optimal sterility (autoclave, sterile fields, etc.) and optimal safety (cardioscope, oxymeter, etc.).
Alopecia with women is different from alopecia with men. It exists in three forms :
1) Alopecia with women after their menopause : this alopecia is spread across the head, but is most obvious at the top of the head.
2) Androgenetic alopecia of the male type : the frontal hairline is driven back. This kind of alopecia is quite rare and it fortunately hardly ever evolves into complete baldness.
3) Androgenetic alopecia of the female type : this is the most frequent form. The hair on the crown of the head becomes thinner, the hairs as such become thinner too and the scalp becomes visible through the hair. The frontal hairline remains quite normal.
Three levels of baldness are usually distinguished, according to the classification of Ludwig.
The extent to which these pathologies can be remedied, depends on the quality and the concentration of the hairs in the donor zone. These must be assessed during the first consultation.

La présence de photos de résultats sur un site internet n’est pas admise par l’Ordre des Médecins en Belgique. Veuillez nous en excuser.
